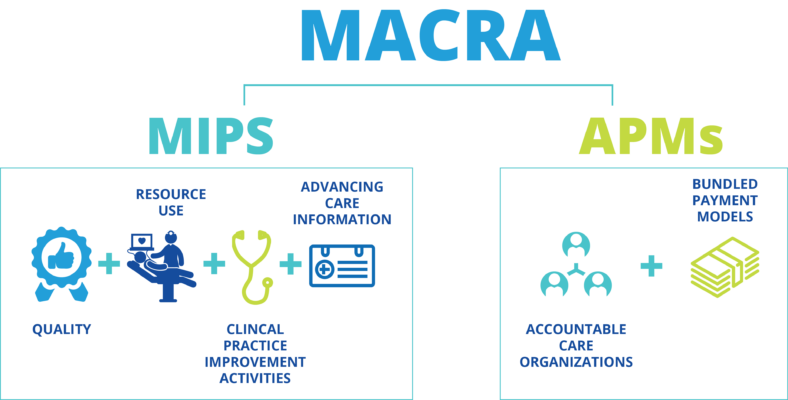
What is MIPS?
Known in full as a merit-based incentive payment system, it’s one of the two programs under the Quality Payment program that moves Part B Medicare providers to a performance-based payment system.
It streamlines the Physical Quality Reporting System (PQRS), The Value-based Payment Modifier Program (VM), and the Medicare Electronic Health Record (HER) incentive program into a single payment program.
MIPS participation
All Part B Medicare providers who meet the MIPS eligible clinician definition have the option to participate as either individuals or part of a group. As an individual, they will report their MIPS data under an NPI number that is tied to one TIN to CMS. Two or more Medicare providers that are eligible and with unique NPIs who have their billing rights assigned to a single TIN can participate in MIPS as a group. As a group, they will also be assessed across all the four MIPS performance categories.
The four MIPS performance categories
MIPS is composed of four performance categories, where performance in each of the four is combined to come up with the MIPS final score, which is then used to determine Part B Medicare payment adjustments in the years to come.
By dividing the performance into categories it helps eligible clinicians have the flexibility to choose the measures and activities that are most meaningful to their practice.
The four performance categories are:
- Quality
It requires eligible clinicians to report data related to the appropriate use of medical resources, patient outcomes, efficiency, patient safety, patient experience, and care coordination to CMS for quality measures. In 2017, it made up 60% of the final score.
- Advancing care information
This category replaces the Medicare EHR incentive program. In 2017, this category made up 25% of the final score. It reflects how well eligible clinicians use EHR technology, with the main objectives being interoperability and information exchange.
- Improvement Activities
Its main intention is to encourage clinicians to participate in activities such as patient safety, shared decision making, coordinating care, and increasing access which in turn improve clinical practice. This made up 15% of the final score in 2017.
- Cost
This replaces the Value-based payment Modifier of CMS and evaluates clinicians on resource utilization which is calculated using Medicare claims. In 2017 it weighed at 0%.
The percentages are based on the percentages of the transition year which was 2017.
Benefits of using MIPS
- It provides monetary incentives.
- It encourages evidence-based treatment.
- You don’t have to re-enter data since the information you initially used is still stored in the database.
- Cash flow is improved.
- The software is easy to use.
- Patient and provider interactions are improved.
Take-aways on MIPS
- Medical professionals who are eligible to participate include, physicians, physician assistants, clinical nurse specialist, nurse practitioners, and certified registered nurse anesthetists.
- MIPS tracking does not mean you fail or pass. Instead, it’s based on what is reported, followed by threshold performance that is compared to your colleagues.
- It doesn’t apply to small practices. It applies to those with more than $30,000 in Medicare charges.
What is APM?
The alternative Payment Model (APM) is a payment approach for paying for medical care that holds Medicare providers responsible for achieving specific performance goals efficiently. They then receive incentive payments. They utilize a reimbursement model as opposed to the fee-for-service model.
The aim is to achieve better quality care without increased spending.
CMS also established a subset of APMs known as Advanced APMs.
What is an Advanced APM?
This is similar to an APM but with some additional criteria:
- EHR technology has to be used.
- It bases payment on quality performances just like those in MIPS.
- Requires entities to bear more than the nominal financial risk for monetary losses.
Participating in an Advanced APM as a QP means you will be exempt from MIPS. A provider’s QP status is calculated using the APM Determination Period.
An APM is considered a MIPS APM if it meets the following criteria:
- The APM entity must participate in the APM under an agreement with CMS or law.
- It must require that APM Entities include at least one MIPS-eligible clinician on a participation list.
- It must not be a new APM for which the first performance period begins after the first day of the MIPS performance year.
- It must not be in the final year of operation for which the APM scoring standard is impracticable.
Here is a list of APMs:
- Comprehensive Primary Care Plus Model
- Primary Care First Payment Model
- Comprehensive ESRD Care Model
- Next Generation ACO Model
- Oncology Care Model
- Vermont All-player ACO Model
To get the incentives the providers must achieve the threshold levels of patients or payments to become qualifying participants (QP).
Qualifying Participants threshold
To become a QP one has to meet two of the thresholds. One for payment amounts and one for the patient count are the thresholds:
- At least 50% of Part B Medicare payments through the advances APM, or
- At least see 35% of its patients through the Advanced APM.
To be considered a partial QP you have to meet the following thresholds:
- Receive at least 40% of its Part B Medicare payments through Advanced APM, or
- See at least 25% of its Medicare Part B patients the Advanced APM.
Clinicians participating in an APM that is not an Advanced APM must participate in MIPS or they will face a penalty. However, those participating in MIPS APMs will receive a favorable MIPS score to reward them for participating in these models.
Since the Sustainable Growth Rate was scraped off, practices must choose from the two reimbursement models. You either choose MIPS or APM. MIPS is closer to fee-for-service but also allows CMS to adjust fees based on scores in efficiency, practice improvement, clinical quality, and meaningful use of electronic health records. Providers are also compared to their colleagues in the same specialty or to themselves to identify how they have maximized resources from one year to another. APM model, however, offers higher reimbursement as per CMS terms. But the risks are greater as physicians who do not meet stipulated metrics are not rewarded with shared savings.
For more information, contact healthcare app development company!